Rethinking Drug Delivery: Innovation to Improve Patient Access to Care
by Mike Hooven, CEO, Enable Injections – LinkedIn published
Consider these facts:
· More than 1 billion IVs are placed each year (1)
· The average time to place an IV is 13 minutes (2)
· More than 1 out of 4 IV attempts fail (3)
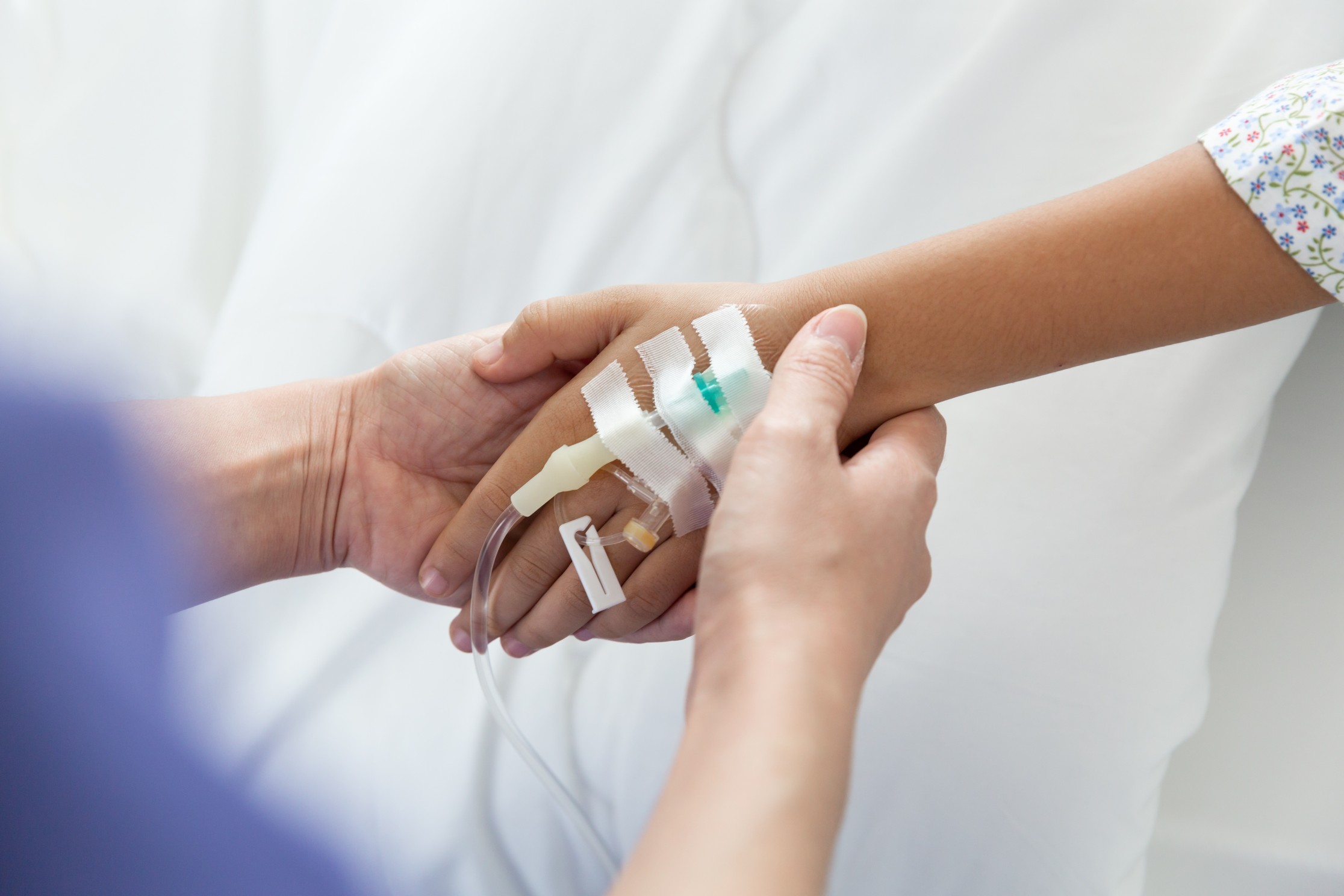
If you have ever received an IV, you understand the significance of IV placement. Rarely does an IV placement go as a patient would want.
In fact, those who regularly receive IVs for treatment tell stories about veins rolling, multiple sticks, alternate access via surgically placed ports, and the pain and anxiety involved when this is all repeated on a routine basis. The health care professional placing the IV also has difficulty – their job is defined by routing large format needles through patients’ skin and into a vein – no small task. But what if there is another way?
Subcutaneous (SC) administration has the potential to change this reality, but not all SC approaches are created equal. With a carefully thought-out approach, many patients receiving IV infusions could have improved access to prescribed treatments.
Safety & Effectiveness: The safe and effective delivery of the therapy is top priority when considering alternatives to IV administration. There is a misconception that larger volumes cannot be administered subcutaneously, except when accompanied by a delivery enhancer. However, additional proteins which claim to enhance SC absorption have been proven to be unnecessary for large volume SC delivery (4), and may expose patients to unnecessary additional proteins without therapeutic benefit. In the majority of scenarios, the right SC delivery means no additional compounds are necessary to accompany a therapeutic to enhance SC absorption or speed up administration.
Versatility: Recent technological advancements promote the delivery of a wider variety of therapeutics and volumes. The right SC delivery system technology not only administers up to 50 mL safely, but also allows the therapeutic to be delivered into SC tissue in a way that may increase comfort and reduce disruption for the patient and provider.
Convenience: IV infusions consume large amounts of time before, during, and after infusion for preparation, administration, and observation. One treatment can take hours out of a patient’s day, and require substantial nurse administration time. However, the right SC delivery provides flexibility for both the patient and provider. With the right SC delivery system, patients will be able to receive their treatments almost anywhere while continuing with daily activities, providing optimal flexibility and convenience.
Impact on Outcomes: Today’s healthcare systems are challenged by a variety of constraints, including human and financial resources. The right SC approach would offer the opportunity for highly skilled health care professionals to focus on the aspects of patient care in which they provide the greatest value, instead of placing lines and monitoring drips. This would have substantial impact on the healthcare system and patient outcomes, with the potential to enhance patient care and manage costs.
Having safe, effective, and flexible options for patients to access the care they need is a priority now more than ever. Don’t you agree?
We look forward to exploring this topic in more detail. Look for more content and perspectives in the coming days and weeks.
References:
1) Beecham G, Tackling G, ‘Peripheral Line Placement’, NCBI. December 1, 2020. https://www.ncbi.nlm.nih.gov/books/NBK539795/
2) Raymond K. ‘Intravenous (IV) Line Access’, International Emergency Medicine Education Project. https://iem-student.org/intravenous-iv-line-access/
3) Lapostolle F, Catineau J, Garrigue B, Monmarteau V, Houssaye T, Vecci I & Adnet F. ‘Prospective evaluation of peripheral venous access difficulty in emergency care’, Intensive Care Medicine. 2007; 33(8): 1452-57.
4) Melissa L, Fadi B, Juneko GO, et al. Assessment of Subcutaneous vs Intravenous Administration of Anti–PD-1 Antibody PF-06801591 in Patients With Advanced Solid Tumors A Phase 1 Dose-Escalation Trial. JAMA Oncology. July 2019; 5(7): 999-1007. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6547134/